Osteoarthritis is a chronic disease of the joints, accompanied by pathological changes of hyaline hyaline, and then in the adjacent tissues, the joint capsule and the synovium.
The lesion is dystrophic and degenerative, which leads to a change in the structure of joint tissues, loss of their functionality. According to the same statistics, 12% of the total population of the planet is susceptible to arthrosis. Between 62% and 65% of all episodes of the disease occur in people over the age of 60.
Another 30-35% of cases of joint damage with this pathology occur in patients aged 40-60 years. And about 3% are young people aged 20-40.
What is this?
In simple words, arthrosis is a chronic disease in which progressive degenerative-dystrophic changes develop in the joint due to metabolic disorders. It is the most common joint pathology, diagnosed in 6-7% of the population. The incidence increases dramatically with age.
Most often, in osteoarthritis, the pathological process includes small wrists (in women 10 times more often than in men), big toe, intervertebral joints of the thoracic and cervical spine, as well as knee and hip joints. Osteoarthritis of the knee and hip joint occupies a leading position in terms of the severity of clinical manifestations and the negative impact on quality of life.
Osteoarthritis is characterized by a complex lesion of the joint and auxiliary apparatus:
- chondritis - inflammatory changes in the cartilage of the joint;
- osteitis - inclusion of basic bone structures in the pathological process;
- synovitis - inflammation of the inner membrane of the joint capsule;
- bursitis - damage to the periarticular sacs;
- reactive inflammation of soft tissues (muscles, subcutaneous tissue, ligament apparatus) located in the projection of the affected joint (periarticular inflammation).
The disease is diagnosed in 2% of people under the age of 45, in 30% - from 45 to 64 years and in 65-85% - at the age of 65 and older. Osteoarthritis of the large and middle joints of the extremities has the greatest clinical significance due to the negative impact on the standard of living and working ability of patients.
Types of osteoarthritis
Depending on the cause of the pathological process inside the joint, there are primary arthrosis, secondary and idiopathic.
It develops primarily as an independent disease, secondarily, as a result of injury or infection, and the cause of the idiopathic form is unknown. In addition to the classification of the disease, depending on the cause of the pathological process, osteoarthritis differs according to the place of destructive changes:
- Gonarthrosis is the most common type of pathology characterized by damage to the knee joint. Gonarthrosis is most often found in people who are overweight, with chronic metabolic diseases in the body and weak immunity. Osteoarthritis of the knee progresses over time and gradually leads to complete loss of motor function.
- Osteoarthritis of the shoulder joint - the main cause of degenerative processes in this area are congenital anomalies in the development of the shoulder joint or excessive stress in this area, for example, when carrying heavy luggage on the shoulders.
- Osteoarthritis - the main reasons for the development of degenerative processes in the ankle joint are trauma, sprains, strains and fractures. In some cases, the development of a pathological process can cause an autoimmune disease - rheumatoid arthritis. Osteoarthritis of the ankle affects dancers, women who wear high heels, athletes.
- Necoarthrosis or arthrosis of the cervical spine - the causes are neck injuries, progressive osteochondrosis, obesity, sedentary lifestyle. At risk are people who work behind a computer in offices. In addition to severe neck pain, patients have severe dizziness, depression of consciousness, impaired memory, and fatigue. These symptoms are caused by compression of the spine, through which nutrients and oxygen enter the brain.
- Coxarthrosis or arthrosis of the ankle - the main cause is changes in the tissues of the joint associated with age. People over the age of 45 are at risk.
- Osteoarthritis of the fingers - develops for the same reason as spondyloarthritis. Polyxarthritis is characterized by damage to several joints with progressive degenerative processes in them, while the pathological process involves ligaments, muscles and tissues surrounding the joint.
- Spondyloarthritis - the tissues of the spine, namely its lumbar region, are susceptible to destructive destruction. Women are at risk during the onset of menopause, as spondyloarthritis progresses due to a lack of female sex hormones.
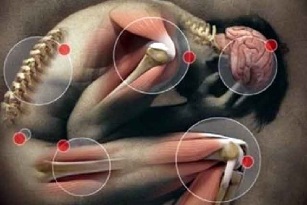
Causes of osteoarthritis
Two reasons contribute to the development of osteoarthritis - stress and lack of adequate nutrition, which provides vitamins and minerals for tissue regeneration. Every person’s joints carry a load. For athletes and dancers during physical work, the load on the legs is higher, which means that the bone joints wear out faster and require quality nutrition. With a quiet lifestyle, the support apparatus wears out more slowly, but also requires periodic tissue renewal.
Therefore, the main condition for the destruction and deformation of the joints is malnutrition, digestion of useful ingredients, which often occurs with metabolic disorders.
List the factors that contribute to joint wear and metabolic disorders:
- Muscle weakness and abnormal joint loading. Weakening of one or more muscles increases the load on the joint and distributes it unevenly within the bony joint. Also, improperly loaded muscles form flat feet, scoliosis, therefore, in these "harmless" diseases, cartilaginous tissues wear out with age, arthrosis occurs.
The likelihood of osteoarthritis increases with strenuous physical exertion.
If daily loads exceed the capacity of bone tissues, microtrauma is formed in them. Thickenings appear at the sites of injury, which over time grow and deform the joint;
- Metabolic disorders (gastrointestinal diseases - bile stasis, dysbiosis, gastritis, cholecystitis, pancreatitis, metabolic disease - diabetes);
- Psychosomatic causes - psychosomatics of arthrosis confirms that a negative emotional state also becomes the cause of the disease. Stress forms muscle spasm, constant stress disrupts the nutrition of all tissues (internal organs, bones, joints);
- Heredity (type of metabolism and its possible disorders are inherited, tendency to muscle weakness or improper formation of the skeletal system, indigestion - which is the basis for the development of osteoarthritis in old age).
Osteoarthritis is a disease of worn joints that has lost a significant supply of minerals and the ability to resist stress and destruction. Therefore, the predisposition to the disease increases with age. After age 70, osteoarthritis is diagnosed in every other retiree. Since the maximum load falls on the legs (a person moves - walks, stands, runs, jumps), here are the first signs of osteoarthritis.
Mechanism of disease progression
When any of the reasons that cause arthrosis of the joint disease appear, pathological processes begin to develop in it. The mechanism of their progression is not fully understood, but the main stages of official medicine are known.
In the initial phase, the structure of the cartilage tissue is depleted and abnormal changes in the synovial fluid. All this happens due to metabolic disorders in which the tissues of the joints do not receive the necessary components in sufficient quantities or some of them are deprived.
Furthermore, the elasticity of collagen fibers and the flexibility of cartilage are lost due to the fact that in a body with a lack of nutrients hyaluronic acid does not have time to produce, which allows the softness and flexibility of the structural composition of collagen fibers. The cartilage gradually dries, becomes brittle and cracks. The fluid in the synovial capsule is gradually depleted and then disappears completely.
Roughness and solid bone growth form on cartilage tissue. At the same time, deformation of other joint tissues, their pathological degeneration, dystrophy and loss of physiological activity develop. For the patient, these changes mean the appearance of pain, lameness, joint stiffness.
Symptoms of osteoarthritis
Acute clinical picture is not typical for arthrosis, changes in the joints are progressive, slowly increasing, which is manifested by a gradual increase in symptoms:
- pain;
- occasional crushing of the affected joint;
- joint deformity that occurs and worsens as the disease progresses;
- stiffness;
- mobility restriction (reduction in the volume of active and passive movements in the affected joint)
The pain in osteoarthritis is annoying transient in nature, it appears when moving, in the background of intense stress, until the end of the day (it can be so intense that it does not allow the patient to fall asleep). The persistent, non-mechanical nature of osteoarthritis pain is not characteristic and indicates the presence of active inflammation (subchondral bone, synovial membrane, ligament apparatus or periarticular muscle).
Most patients notice the presence of so-called initial pains that occur in the morning after waking up or after a long period of inactivity and pass during physical activity. Many patients define this condition as the need to "develop a joint" or "break it. "
Osteoarthritis is characterized by morning stiffness, which has a clear localization and is short-lived (no longer than 30 minutes), and patients sometimes perceive this as a “wanting feeling” in the joints. Feeling of wedge, stiffness is possible.
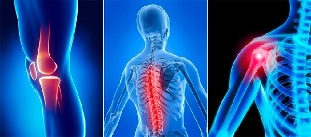
With the development of reactive synovitis, the main symptoms of osteoarthritis are joined by:
- pain and local fever, determined by palpation of the affected joint;
- persistent pain;
- joint enlargement, soft tissue swelling;
- progressive reduction of range of motion.
Stages and degrees of arthrosis
During the course of the disease, medicine distinguishes three stages that differ in the signs of the disease, the intensity of the lesion and the localization. At the same time, the differences in all three stages refer to the types of tissues in which pathological changes undergo.
- The first stage of the development of arthrosis of the joints is the initial stage of the disease. They are characterized by mild damage to cartilage tissue and loss of physiological functions in collagen fibers. At the same time, in the first phase, minor morphological disorders of bone tissue and structural changes of synovial fluid are observed. The cartilage of the joint is covered with cracks, the patient has a slight pain at the site of pathology.
- Second degree - development of arthrosis with increased dynamics. This phase is characterized by the appearance of stable pain, lameness. Morphological and dystrophic changes are noticeable in the cartilage; During diagnosis, bone growth is detected. Osteophytes are formed - bone growths that are visible during the visual inspection of the lesion site. At the same time, the processes of degenerative changes of the synovial capsule take place, which leads to its structural depletion. The disease at this stage can often get worse and be regular. The pain gradually becomes permanent.
- Third degree - active progression. At this stage, the synovial fluid is almost completely absent due to its degeneration, and the bone tissue rubs against each other. Joint mobility is almost completely absent, the pain becomes more palpable. Cartilage is also absent due to degenerative and atrophic changes. Treatment of third degree arthrosis of the joints is considered inappropriate.
In addition to these three stages of pathology development, there is a final stage - the irreversible destruction of all joint tissues. At this stage, it is impossible not only to carry out effective therapy, but even to alleviate the pain.
The inflammatory process usually begins in the second degree of the lesion, in rare cases, in the absence of medical intervention - in the first stage. After that, it is increasingly difficult to stop it, and this can lead to secondary pathologies, the development of pathogenic microflora at the site of disease localization.To rule out severe consequences, treatment should be started from the first stage, and intensive therapy methods should be applied at the same time. In the last phase, associated with the complete destruction of cartilage tissue, only one technique is allowed by which the patient is relieved of pain and immobility of the joint - arthroplasty by complete or partial replacement of the components of the joint.
Consequences
The consequences of untimely treatment and advanced arthrosis of the joints abound in complications such as:
- Disability;
- deformation after recovery;
- occurrence of vertebral hernias;
- stiffness or stiffness of the joint;
- decline in quality and standard of living.
The chronic course, in addition to these complications, is accompanied by intense and frequent pain, complete destruction of the structural components of the joint, discomfort, inability to work physically and play sports.
Diagnostics
The diagnosis of arthrosis is based on the assessment of anamnestic data, characteristic manifestations of the disease, the results of instrumental research methods. Indicative changes in general and biochemical blood tests are not typical of osteoarthritis, but occur only with the development of an active inflammatory process.
The main instrumental method for diagnosing osteoarthritis is radiography, and in diagnostically unclear cases, computation or magnetic resonance imaging is recommended.
Osteoarthritis of the knee and hip joint occupies a leading position in terms of the severity of clinical manifestations and the negative impact on quality of life.
Additional diagnostic methods:
- atraumatic arthroscopy;
- ultrasonography (assessment of articular cartilage thickness, synovium, joint capsule condition, fluid presence);
- scintigraphy (assessment of the condition of the bone tissue of the bone heads that make up the joint).
How to treat osteoarthritis?
Arthrosis of the joints is better treated at an early stage, the treatment itself should be pathogenetic and complex. Its essence lies in eliminating the causes that contribute to the development of this disease, it is necessary to eliminate inflammatory changes, and restore functions that were previously lost.The treatment of osteoarthritis is based on several basic principles:
- Oxygenation of the joint, or so-called intra-articular oxygen therapy.
- Drug therapy.
- Intraosseous blockages as well as metaepiphysis decompression.
- Sustainable diet.
- Damaged joints must be relieved of excessive stress. If possible, it should be kept to a minimum during treatment
- Follow the established orthopedic regimen.
- Physiotherapy exercises.
- Taking a physiotherapy course, which includes magneto and electrotherapy, shock wave and laser therapy.
- Sanatorium treatment. To do this, it is necessary to undergo a course of treatment in specialized resorts once a year, on the recommendation of a doctor.
Preparations for the treatment of osteoarthritis
Drug treatment is carried out in the phase of exacerbation of osteoarthritis, and is selected by a specialist. Self-medication is unacceptable due to possible side effects (for example, the negative effect of nonsteroidal anti-inflammatory drugs on the gastric mucosa).
Therapy includes the following drugs:
- Anti-inflammatory drugs. By starting arthrosis therapy in a comprehensive way, you can slow down the course of the disease and significantly improve the quality of life. It is worth inquiring in more detail about some points of treatment. In particular, drug therapy involves the initial stage - it is the removal of pain, as well as the removal of inflammatory processes that occur in the joints. For this, all doctors use nonsteroidal anti-inflammatory drugs. Experienced doctors do not recommend taking them orally because these drugs irritate the stomach wall to a greater extent. Therefore, depending on the drug selected, it is used either intravenously or intramuscularly. NSAIDs in the form of ointments are sometimes used as adjuvants, but their absorption is extremely low, so a significant effect cannot be achieved.
- Hormonal corticosteroids. When the arthrosis is in the phase of worsening, it is desirable to take hormonal corticosteroids. They are injected into the wrist. You can use a special plaster, ointment or tincture on the outside, which is made on the basis of hot peppers.
- Chondroprotectors aimed at restoring cartilage and improving the qualitative composition of synovial fluid will not be superfluous. The course lasts quite a long time, until the moment when there is an improvement. However, if the expected effect does not appear within six months of use, the medication should be discontinued. It is also recommended to use drugs made on the basis of hyaluronic acid intraarticularly, together with chondroprotectors. They contribute to the formation of the cell membrane that is responsible for the formation of articular cartilage.
Physiotherapy
To relieve pain, reduce inflammation, improve microcirculation and relieve muscle cramps, a patient with osteoarthritis was referred to physiotherapy:
- In the deterioration phase. Prescribe laser therapy, magnetotherapy and ultraviolet radiation
- In remission. Electrophoresis and phonophoresis shown.
In addition, thermal processes, sulfide, radon and marine baths are used. Electrical stimulation is performed to strengthen the muscles. Gentle massage can also be used during remission.
Surgery
If the above methods of exposure are ineffective, in the presence of complications resort to surgical treatment of osteoarthritis:
- Decompression of the metaepiphysis and prolonged intra-axial block (reduction of intra-axial pressure in the affected area);
- Corrective osteotomy;
- Endoprosthetics of joints.
In the early stages of the disease, mechanical, laser or cold plasma removal is used (smoothing the surface of damaged cartilage, removing inanimate areas). This method effectively relieves pain, but has a temporary effect - 2-3 years.
Folk remedies
Most people these days don't want to take pills or injections. Therefore, the question arises - how to cure osteoarthritis with the help of folk remedies? For the most part, such funds are aimed at increasing tone in the body, improving blood circulation, relieving pain and increasing immunity.
Traditional medicine recipes are used to treat this disease:
- The egg solution is made from fresh egg yolk, which is mixed with turpentine and apple cider vinegar in a ratio of 1: 1: 1. The liquid must be thoroughly mixed and wiped over the affected joint overnight. Then you need to wrap everything in a woolen scarf. It is recommended to rub for 1 month 2-3 times a week.
- Buy elecampane root from a pharmacy. As a rule, it is packed in packages of 50 grams. To prepare the tincture you will need half a packet of the root of the plant and 150 ml of high quality vodka. The ingredients are mixed, placed in a dark bottle and infused for 12 days. Rubbing is done before bedtime and, if possible, in the morning.
- Using cooked oatmeal also gives good results. Take three to four tablespoons of oatmeal, pour over boiling water and cook on low heat for five to seven minutes. The amount of water used should provide a thick paste, which should be cooled and used as a compress overnight. Use only freshly cooked flakes. Yesterday's porridge is not good for compresses.
- Birch leaves, nettle leaves and marigold flowers are taken in equal parts. As a result, you need to get two tablespoons. Put the resulting crumpled collection in a thermos, pour a liter of boiling water and leave overnight. The next morning, four to five times a day, you should take half a glass of soup. The course of taking this recipe is two to three months.
Tinctures of bay leaves, horseradish, garlic and rye grains are also considered effective. Treatment of osteoarthritis with folk remedies will be most effective if combined with drugs.
Diet for osteoarthritis
The basic principles of nutrition for osteoarthritis are as follows:
- Avoid heavy meals at night to avoid osteoarthritis.
- Eat fractionally.
- Constantly control your weight, to avoid weight gain,
 and, therefore, additional stress on painful joints.
and, therefore, additional stress on painful joints. - When the disease does not get worse, take a walk after eating.
- The menu must be balanced, compiled with a doctor.
There are no complaints about fish dishes - you can eat a lot of them, of course, in reasonable quantities.
- Don't forget to take your vitamins regularly from food. B vitamins are especially relevant for patients with arthrosis
- Deer meat plays an important role in the treatment of osteoarthritis. Such food will be a real storehouse of trace elements for inflamed joints. The most important component of aspic is collagen found in nature
- Vitamin B helps produce hemoglobin. It can be "obtained" by eating bananas, nuts, cabbage and potatoes. It is worth taking away the herbs and legumes. They will be a source of folic acid. Liver, mushrooms, dairy products as well as eggs will be helpful. They are rich in riboflavin.
Following a treatment regimen prescribed by a doctor, it is possible to get the disease to go away and the damaged tissue to start regenerating.
Prevention
Prevention of osteoarthritis begins with proper nutrition. You should try to reduce your intake of salt as well as foods that can disrupt your metabolism. These include legumes, fatty meats and alcohol. The diet includes cabbage, greens and fish.
For the prevention of arthrosis, it is necessary to attend physical education classes, do warm-ups. If possible, it is better to walk a few kilometers. It is also important to monitor your weight and prevent weight gain, as this will put extra stress on sore joints. It is not recommended to take pills for the purpose of losing weight, because they can disrupt the metabolism in the body.
Forecast
The outlook for life is favorable. The benefit of social and work prognosis depends on the timeliness of diagnosis and initiation of treatment, it decreases if the decision on the issue of surgical treatment of the disease is delayed.





































